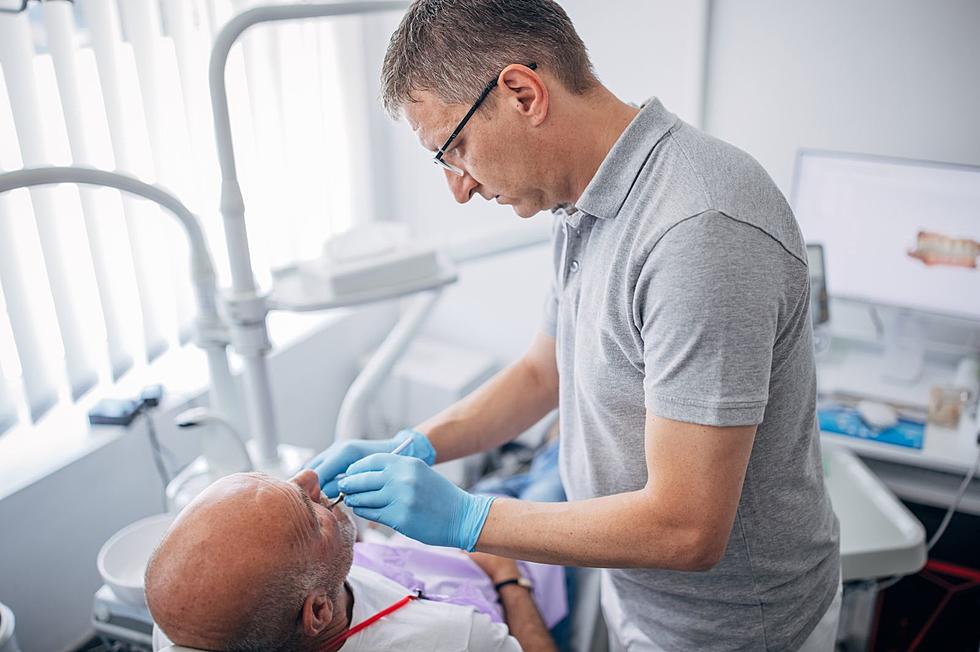
DiNapoli Finds Errors in Medicare, Medicaid Billing Costing NY $26m
The State Department of Health made $26 million in Medicaid over payments and other questionable payments because of flaws in its e-Med NY claims processing computer system, according to an audit released by State Comptroller Thomas DiNapoli.
The audit looked at claims for patients who are both Medicare and Medicaid eligible, which are known as crossover claims. In December 2009, the Department of Health implemented a new payment mechanism in e-med NY to achieve greater control over Medicaid payments.
The new tool is an attempt to ensure Medicaid does not pay crossover claims denied by Medicare, only pays the portion of the claim that it actually owes and crossover claims are billed first to Medicare before being billed to Medicaid.
DiNapoli’s auditors found that from implementation of the new system in 2009 through March 31, 2012, the system was not working correctly, allowing nearly 866,000 improper and questionable payments to be made.
More From CNY News